Donating bone marrow in Germany: My boyfriend's experience
I know, it's been ages since I've blogged. I haven't forgotten about this; I just got so caught up in my first year of grad school that it was terribly difficult to find the motivation and the time to sit down and blog consistently. This marks the first of my efforts to re-enter the 'blogosphere.'
Recently, my boyfriend had the experience of donating bone marrow to a stranger as facilitated by his registration with the DKMS, Germany's national bone marrow donation registry. Given that this is a process about which many people still seem to have misconceptions (based on the number of times people told us, "oh, I could never do that – I heard it's very painful!"), I wanted to write a blog post about his experiences to shed some light about what donating bone marrow in this day and age actually means. Though his experiences are specific to donating in Germany, I am guessing the process is very similar to what it would be in other countries (especially given the fact that donations are not restricted to people located in your same country, as you will see in this post).
In February of this year, my boyfriend Paul registered himself with the DKMS. One of his bosses had encouraged him to do it, and since the process is so straightforward, there wasn't really a good reason not to. He filled out the questionnaire online, and within a few days a cotton swab kit was sent to our apartment so he could provide the registry with a DNA sample. He completed that part and sent it back to their laboratory, promptly forgetting about the whole thing. Many people register themselves for organizations like this but are never matched with any patients – why should Paul be any different?
1. Finding out about the match
Except, he was. Remarkably different, in some regards – within a month of registering (so, at the beginning of March), Paul received a letter in the mail informing him he was a possible match for someone. The DKMS asked him to please call them as soon as possible to discuss next steps.
He called and learned more about what the current situation was. They informed him that based on the DNA information they already had from him, there was an 80 percent chance that he was indeed a matching donor for someone. Once establishing that he was still willing to be a possible donor, they arranged a doctor's appointment for him the following week to get additional bloodwork done.
We also learned a bit more about how the possible future donation would work. There are two main ways people donate bone marrow: the first and by far most common procedure is called "peripheral blood stem cell transplantation" (PBSCT); it is akin to donating plasma -- the entire donation is done via a needle in one arm that draws the blood out and into a machine that separates the stem cells (or something like that, I'm no expert) and then cycles the rest of the blood back into your body via a needle in your other arm. This is the donation procedure in 80 percent of cases. The less common procedure involves what I think is many people's classical conception of how donating bone marrow works, as it involves inserting a needle into your pelvic bone to draw the bone marrow out directly (this is where I think many people get the idea that bone marrow donation is very painful, even though this procedure would be done under full anesthesia).
One important point to stress here is how heavily consent-based the entire process is and how much of an emphasis there is on this being a choice that you are free to make or not make. This was something Paul heard constantly during this process -- he had no obligations to continue and could back out at any time for any reason with no questions asked.
His doctor's appointment was largely uneventful. His blood samples were sent off for further analysis to confirm the match, and we waited to hear what the final verdict was. Just over three weeks later, Paul received the call: he was indeed a match for someone, and if he was still interested, he could potentially save someone's life with his donation.
2. The donation process -- preparations and day-of
Well, of course he was still interested. Donating bone marrow is not a trivial process, but neither is it deeply invasive and life-altering. What they explained to Paul was that he would be donating via the more common method, PBSCT. In the week before his procedure, he would need to give himself regular injections to boost the number of stem cells present in his blood. These injections would likely have side effects similar to having the flu, i.e. a general sense of unwellness, but these effects would quickly subside after the donation.
The donation was scheduled for the beginning of May, so there was roughly a 4-week span between when he found out he was a definite match and the actual donation. About three weeks before the procedure, he went to the clinic that was overseeing the donation for a pre-check to make sure he was healthy enough to proceed. One important part of this check was making sure his spleen was normal, since apparently the drugs involved in increasing stem cell production could cause a temporary enlargement of the spleen, which could have particularly negative health impacts on a spleen that is not otherwise healthy. He had no issues during his pre-check, so the donation remained scheduled for a few weeks later. During this visit, he also received the medication he would need to be injecting prior to the procedure.
Five days before the donation, Paul began his injections. It was a relatively simple process -- a double dose in the morning, single dose in the evening -- and while giving yourself a shot is probably never fun, he did it dutifully and without complaints. The injection site was his stomach.
Initially, he didn't seem to have much of a reaction to the drugs, but after a few days he definitely became more fatigued. He complained frequently of general internal discomfort (less about being in pain and more about it being a very odd or unsettling feeling), and in particular became acutely aware of where in his body his spleen was located, which many people probably cannot say. Occasionally, his spleen would "pulse" in a painful way, although it was always short-lived. While he was still able to function normally during the period right before the donation, suffice to say he was very ready to be done with it all by the time the date rolled around.
Around this time, Paul's recipient was undergoing intensive chemotherapy treatment to kill cancer cells as well as suppress the recipient's immune system in preparation for the transplant. Because of this, it is extremely risky for the patient if a donor backs out on a donation late in the game. Paul could still back out any time he wanted, but the DKMS did let him know that the risks to the patient from him backing out would increase -- to the point of being life-threatening -- the further into the process he got.
The night before the donation, Paul traveled down to Dresden, where the clinic he was donating at was located (Dresden is home to a much larger facility than the one in Berlin, so he was assigned there). I could have come with, but unfortunately I had to work. At this point, we still did not know anything about the person he was donating to -- not their age, not their sex or even their medical condition. This is to protect the patient's privacy, but also to ensure Paul retained full agency in his decision to donate -- it probably would be much harder to say no to a donation if you knew it would be for a 12-year-old child, for example.
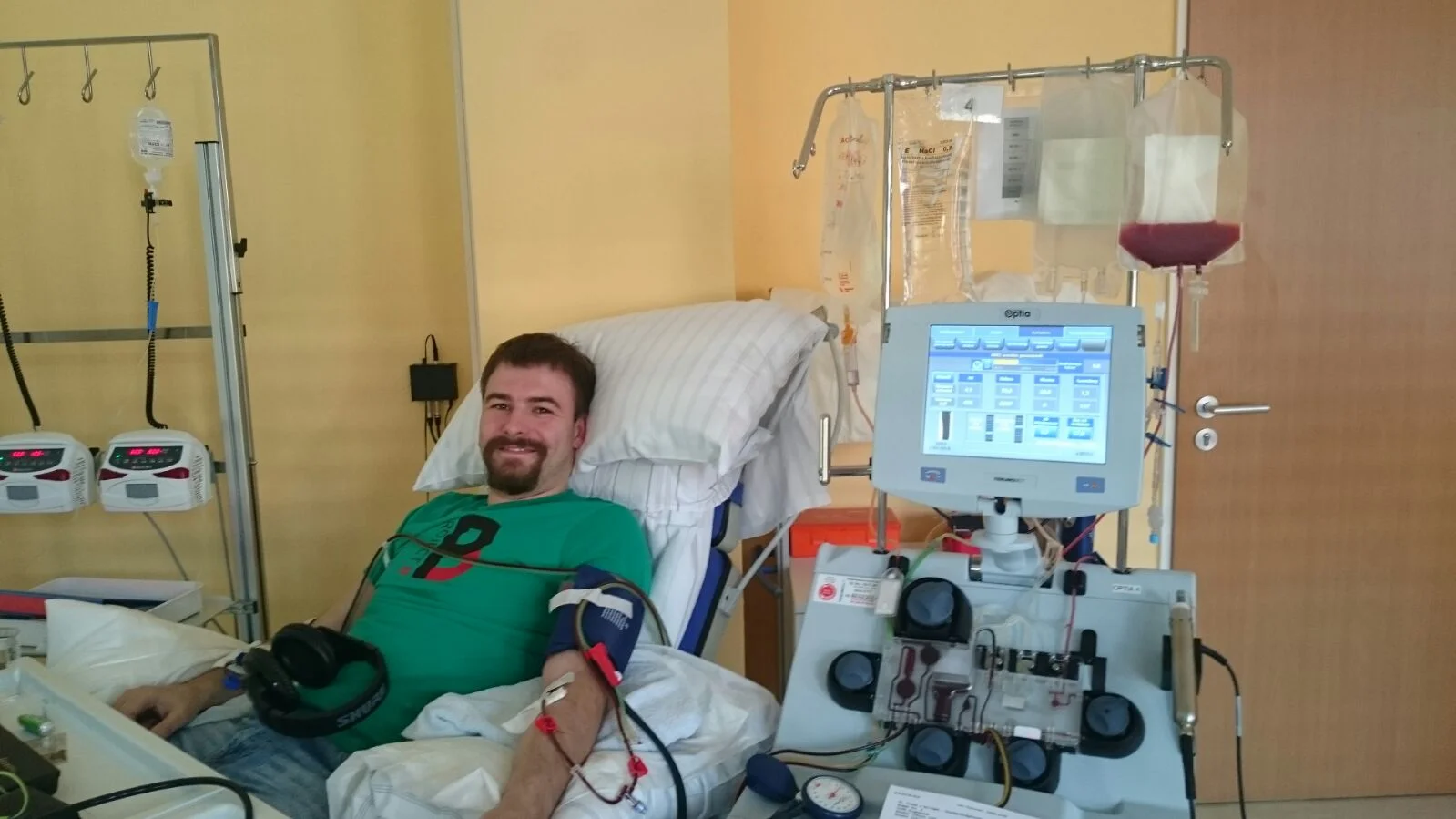
On the following morning, Paul reported to the clinic to begin. By 8 a.m., he was hooked up to the machines and settled in. He had his phone with him during the process, and they also provided movies to watch. It wasn't certain at first if they would get everything they needed in one day, or if he would need to come back for a second day. But by 2 p.m., he was finished up and they decided they had what they needed. He was free to catch the next train back to Berlin, closing a chapter on this two-month journey.
Paul during his donation
3. Post-Donation
The following day, Paul had the chance to call the clinic to learn a little bit more about the person he donated to. To my surprise, we learned that his recipient was a middle-aged American. I had no idea that the registries were so international, and that there was even a chance that the person he was donating for was not on the European continent. Paul's actions potentially saved not just the life of a stranger, but the life of a stranger several thousand miles away from him. Take a second to marvel at how amazing living among the connectedness of the 21st century is.
As far as recovering from the procedure, Paul was fit to come visit me at work and drink a beer just a few hours after leaving the clinic (although perhaps a post-procedure beer would not be recommended by a medical professional). He had no lasting side effects from the procedure and quickly regained his normal energy levels.
As far as contact between the donator and the recipient, for now it is radio silence. In about three months (totaling four months after the procedure), we expect that we will get an update from the American clinic on how the recipient is doing. Beyond that, we will have to wait two years before either side is allowed to initiate non-anonymous contact (there is the possibility to initiate anonymous contact any time between now and then, but Paul would prefer to only do that if the patient chooses). The idea behind this two-year waiting period is to ensure non-anonymous contact only begins after the likelihood of the cancer returning is extremely low -- again, the concern is for making sure that if Paul were to be called upon once more to donate to this patient, that he would retain full agency of the decision and not be swayed by any emotional contact to the patient.
4. Join In
If you live in Germany, please consider joining the Deutsche Knochenmarkspenderdatei. I did shortly after Paul's donation. Their website is available in German, English and Turkish.
If you live in the U.S., please consider joining the Be the Match Registry or the DKMS (I recently learned they have a US branch).
For both registries, the registration process is simple and requires minimal effort on your behalf.
Moreover, after this blog post, I hope more people understand what the process of donating bone marrow for a stranger is actually like (or at least, what it is like for approximately 80 percent of such cases) and thus that fewer people will lean on the excuse of "oh, registering is such a great thing to do, but I don't think I could ever endure the donation process myself." In our case, I think it was absolutely worth it. The DKMS was a great organization to work with. They kept Paul constantly informed about what was happening and what he could expect as next steps, made themselves available to him to answer any questions that came up, and also made sure he was fully informed of his rights as a donor. Moreover, the temporary discomfort involved in preparing for the donation pales in comparison to the fact that somewhere across the Atlantic, there is a family that has renewed hope for the life of their father, brother, son, uncle or cousin.
I hope that two years from now, I can write a blog post about Paul finally getting to meet that man. Until then, I wish this stranger all the best and hope Paul's donation is enough to help him pull through.